|
11/29/2023 0 Comments Ibs vs crohns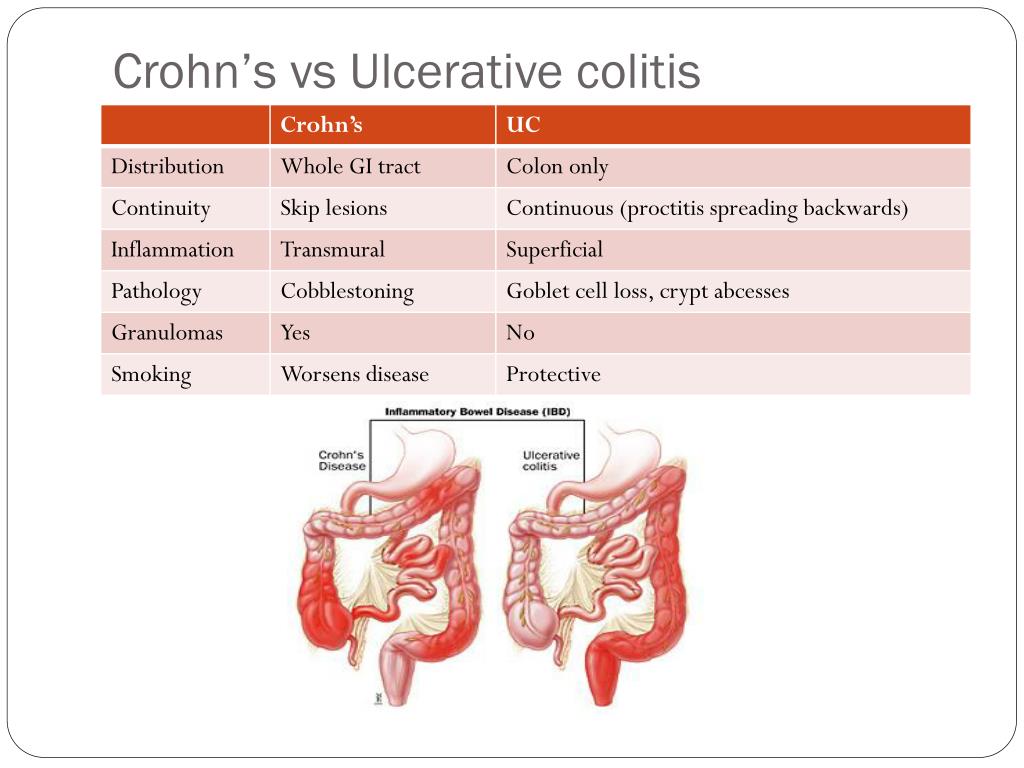
A more likely explanation is that IBS was present first (remember it is very common) and the IBD started later.įinally, both IBD and IBS may be mistaken for other diseases such as appendicitis, diverticulitis, and chronic gut infections. There are many reported instances where IBD has been “misdiagnosed” as IBS for years until finally the diagnosis is made. The powerful, often expensive, sometimes-toxic drugs employed to treat IBD will not improve IBS symptoms. It is therefore crucial that the IBS symptoms in these patients not be confused with those due to IBD. That is, they may occur in the same patient due to chance. Because so may people have IBS, it is not surprising that some will also acquire IBD. There are other important considerations. While both are chronic, the overall treatment and prognosis are very different. It is of vital importance to distinguish these two very different gut conditions. None of these terms is entirely satisfactory. While IBD is described as a structural or “organic” disease, IBS is said to be functional or a disorder of function. While many people with IBS complain of social inconvenience, embarrassment, fear of appearing in public, and work loss, these features are more universal and profound in IBD, as the foregoing comparisons imply. 
However, there is little evidence that this is true of IBS overall, and psychosocial difficulties are found in some people with IBD as well. Certainly, some patients who seek medical attention may also have psychosocial problems that require attention in their own right. Sometimes psychological disease is thought to be a part of IBS. While neither condition will shorten life expectancy, most of those with IBD will require surgery at some time during their illness. None of these physical disabilities result from IBS, and having IBS does not predispose one to IBD, nor any other structural condition such as cancer, celiac disease, nor diverticulosis. The resulting dermatitis, arthritis, and iritis (red, sore eye) can be as debilitating as the IBD itself. In IBD, inflammation may occur beyond the gut in the skin, joints, and eyes for examples. 
However, the structural damage of IBD may produce striking physical findings such as a mass in the abdomen, an abnormal communication of the gut with the skin (fistula), an anal abscess, or the physical features of weight loss and anemia. There are no findings on physical examination that are characteristic of IBS. The inability to eat during attacks, and wasting of energy caused by the inflammation, result in weight loss and malnutrition. The disrupted intestines may bleed and anemia (low blood) is common. This damage is resisted by the body’s defences, resulting in fever and malaise. In IBD, the gut is damaged by the chronic inflammation. More than half of people who have IBS symptoms seek no medical attention, while few IBD sufferers can avoid it. IBS appears to be a worldwide disorder, while IBD prefers the planet’s temperate zones. 
IBD has no gender preference and is most common in Jewish individuals and those with origins in Northern Europe. Females are more likely to have IBS, and it affects all races. Demographicsīoth affect people of all ages but they are particularly prominent in young people. We know IBS exists because patients have gut symptoms, and there is no other way to detect it. Examination of the gut of a person who has IBS will be unrevealing. In IBD, this damage is caused by an inflammation whose origins are poorly understood, but whose consequences may require hospitalization, heavy-duty medication, nutritional support, and often surgery. By “structural,” we mean that when we examine the gut by x-ray, endoscopy, surgery, or biopsy we can see structural damage to the gut. The fundamental difference between IBS and IBD is that IBD is structural, and IBS is not. For many reasons, which are not relevant to this discussion, these two inflammatory conditions are usually lumped together as IBD. The former affects only the lining of the large intestine or colon, while Crohn’s disease may affect any part and all layers of the gut. To add to the confusion, “IBD” is used to describe two distinct, but different structural diseases: ulcerative colitis and Crohn’s disease. It is unfortunate that the initials for these contrasting conditions are so similar. However, about the only features that they have in common are gut symptoms such as abdominal pain and diarrhea, a tendency to affect young people, chronicity, and our ignorance of their ultimate cause. Both are very common illnesses that affect the gut. People can be forgiven if they confuse irritable bowel syndrome (IBS) with inflammatory bowel disease (IBD).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
